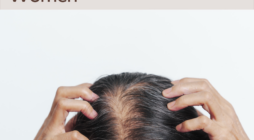
Polycystic ovary syndrome (PCOS) is among the most common hormonal conditions in women of reproductive age. Beyond irregular periods, acne, and metabolic issues, many experience hair thinning that affects confidence and day-to-day life. A key cause of hair loss in PCOS is excess androgens—often called male hormones—and the downstream formation of dihydrotestosterone (DHT). This page explains how PCOS drives hair changes, typical symptoms of PCOS around the scalp, and evidence-based medical treatments that can support better hair health and hair growth.
What Is PCOS?
PCOS is a hormonal disorder characterized by:
- Hyperandrogenism (elevated levels of testosterone or clinical signs of androgen excess)
- Ovulatory dysfunction (irregular or absent cycles)
- Polycystic ovarian morphology (multiple small follicles on ultrasound)
Metabolic features—such as insulin resistance and altered insulin levels—are also common and can amplify androgen production, contributing to scalp changes and weight gain. Strategic lifestyle support (including sustainable weight loss) complements clinical care.
How PCOS Leads to Hair Loss: Androgens & DHT
Androgen Excess in PCOS
In PCOS, circulating androgens (e.g., testosterone, androstenedione) may be elevated or more active at the follicle level. Even when labs are “normal,” heightened follicle sensitivity can still drive miniaturization. A case-control study of women with androgenic alopecia reported polycystic ovarian morphology in 67% of cases versus 27% of controls, alongside higher androgen markers and free androgen index.1
DHT and Follicle Miniaturization

Testosterone converts to DHT via 5-alpha reductase; DHT binds androgen receptors in susceptible follicles, shortening growth phases and reducing shaft diameter. Over time this resembles female pattern hair loss, particularly at the crown and part line.
Evidence from Clinical Research
Reviews link hormonal imbalance, metabolic alterations, and hair-cycle disruption in PCOS.2 Dermatology guidance recognizes PCOS as a leading endocrine driver of hair loss and encourages early diagnosis and treatment to improve outcomes.3
Symptoms & Patterns
- Diffuse thinning over the crown/temples, widening of the central part
- Increased shedding out of proportion to routine stressors
- Co-features of hyperandrogenism (acne, oily skin), cycle irregularity
Unlike postpartum shedding, which is temporary, PCOS-related thinning tends to persist without directed care.
Diagnosis
A proper workup helps tailor care and rule out co-factors:
- Blood tests: total/free testosterone, androstenedione, DHEA-S, SHBG
- Pelvic ultrasound for ovarian morphology
- Exclude thyroid disease, nutritional gaps (e.g., iron deficiency) and autoimmune causes
Treatment Options
Lifestyle Foundations
- Nutrition patterns that support insulin resistance and stable insulin levels
- Gradual, sustainable weight loss where appropriate
- Stress management and sleep optimization
Medications & Topicals
- Topical minoxidil for promoting visible hair growth
- Anti-androgens (specialist-guided): spironolactone; 5-alpha-reductase inhibitors in select cases
- Hormonal modulation via birth control (combined birth control pills may reduce ovarian androgen output)
Therapy choice depends on the underlying cause, goals, and safety profile; discuss potential side effects and monitoring with a clinician.
Nutrition & Adjuncts
- Correct low ferritin/iron deficiency with appropriate iron supplements
- Consider inositol for metabolic support in PCOS
- Botanical options with early data on DHT modulation (e.g., saw palmetto)
Procedural Therapies
- PRP (platelet-rich plasma) to stimulate follicles
- Exosome treatments (emerging/regenerative)
- Hair transplant in stable candidates with adequate donor supply
Early intervention and combination approaches (e.g., minoxidil + anti-androgen + lifestyle) typically yield the most reliable improvement trajectory.
Prognosis
With consistent care, visible improvements often appear over 6–12 months and generally require maintenance. For fundamentals on DHT, see: What Is DHT? For mindset and support, see: Confidence Restored.
FAQs
Can PCOS hair loss be reversed?
Many women improve with consistent, multi-modal care. Outcomes depend on severity, timing, and adherence to a plan that addresses hormone and metabolic drivers.
Which doctor should I see?
Start with your primary care or OB-GYN; dermatology and endocrinology input can refine medical treatments based on labs and goals.
Is hair transplant an option for PCOS?
In select, stable cases with adequate donor supply, it can complement medical therapy. Ongoing management of hormonal drivers remains essential.
References
- Cela E, Robertson C, Rush K, et al. Prevalence of Polycystic Ovaries in Women with Androgenic Alopecia. PubMed
- Moini A, et al. Pathophysiology and treatment of polycystic ovary syndrome: An overview. PMC
- Borda LJ, Perper M, Keri JE. Polycystic ovary syndrome and its dermatologic manifestations. JAAD